Should Catheter Leak? A Home Troubleshooting Guide
Learn urgent, practical steps to diagnose and safely address a catheter leak at home. Quick fixes, safety tips, and when to consult a clinician.
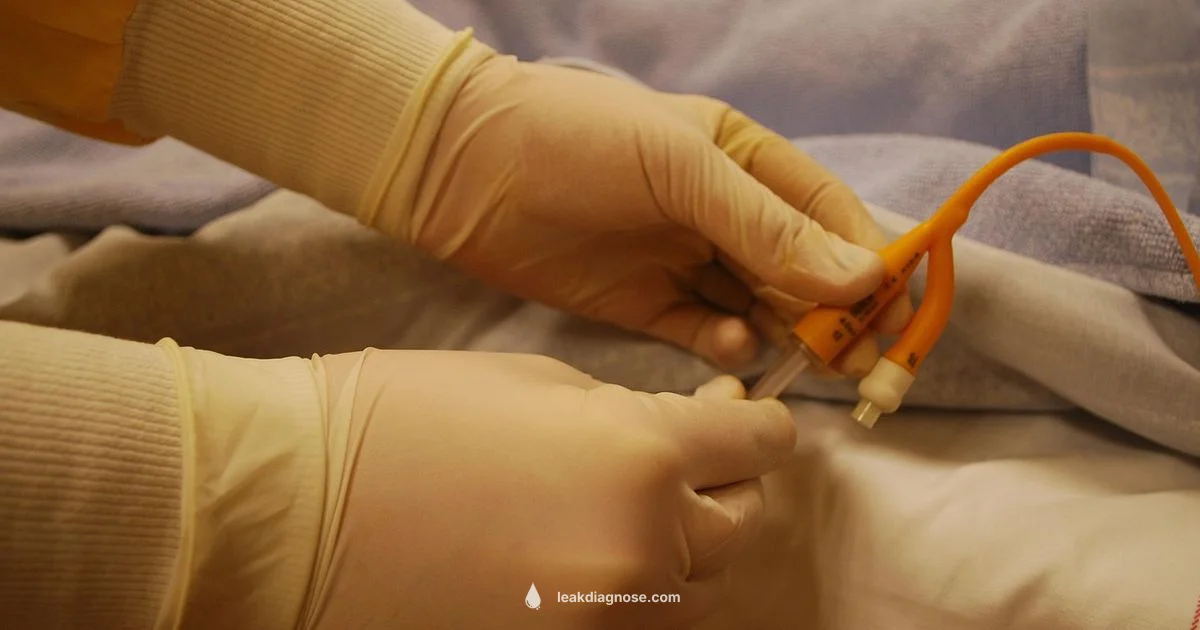
Most catheter leaks come from a loose connection or a kink in the tubing. Start by inspecting the catheter and tubing for kinks, confirm that the drainage bag is connected securely, and check the retention balloon is inflated to the recommended volume. If leakage continues after these checks, seek medical advice promptly.
Should catheter leak indicators and why they matter
A leak around a urinary catheter is not just an annoyance; it can signal a breakdown in the closed system that protects the bladder from infection. In home care, leaks may occur at the catheter-to-tittings junction, along the tubing, or from the drainage bag if fittings aren’t sealed. Recognizing the origin helps you respond quickly and protect your health. The phrase should catheter leak often appears in clinical guidance to describe when to probe for the weakest link in the setup. Early action reduces skin irritation and infection risk, and it keeps the drainage pathway clear for accurate monitoring. If you notice fever, unusual urine color, or foul odor, treat as urgent and contact your clinician or emergency services as appropriate. Always document the time and the exact location of the leak to share with a healthcare professional.
Common causes of catheter leaks in home care
Leaks aren’t uncommon in the first days after catheter insertion, but most are fixable with careful checks. Common causes include loose connections at the catheter or bag junction, kinks or pinches in tubing, and balloon-related issues (underinflation, overinflation, or a damaged balloon). In some cases, dislodgement or improper securement at the insertion site can create a gap for leakage. A faulty drainage bag clamp or a clogged line can also lead to seepage. By noting where the leak originates—at the connection, along the tubing, or near the balloon—you can guide your clinician with precise details. The goal is a tight, unobstructed flow that keeps urine where it belongs.
Immediate steps you can take safely
If you notice a leak, begin with simple, non-invasive checks. Wash your hands and gather supplies. Inspect every connection for a secure fit and tighten gently if needed. Look for kinks or bends in the tubing and reposition so the line runs smoothly. Ensure the drainage bag is properly attached and positioned below bladder level to promote gravity-driven drainage. Confirm the retention balloon has the correct inflation volume as instructed by your clinician, using sterile technique if required. Do not apply heat, force, or heavy tension on any part of the system. If the leak persists after these steps, document what you see and contact your clinician immediately. In case of fever, severe pain, or rapid deterioration, seek urgent care right away.
Diagnostic flow: symptom → diagnosis → solutions
A practical flow helps you decide when home care is appropriate or when to escalate. Start with the symptom: a visible leak around the catheter or seepage at the connection. Next, test likely causes: is the bag firmly attached? Are there obvious kinks? Does the balloon hold air? If basic checks fail, the likely diagnosis may be a damaged catheter or a malfunctioning balloon, which requires professional replacement. Solutions range from re-connecting and tightening fittings to replacing the catheter under supervision. Always defer to your clinician for confirmation before making any permanent changes to the device.
Step-by-step: Fixing the most common leak
- Inspect all connection points between the catheter, tubing, and bag; ensure tight, clean connections. Tip: wipe with an alcohol wipe before reconnecting to reduce bacteria risk.
- Look for kinks or bends in the tubing; straighten and reposition so the line runs smoothly without pressure points. Tip: keep tubing loosely coiled in a gentle arc rather than a sharp bend.
- Recheck the bag position; ensure it is below bladder level and not tugged on the catheter. Tip: use a stable holder or stand.
- Verify balloon inflation to the prescribed volume with a sterile syringe; if you cannot confirm, contact your clinician before proceeding. Tip: never overinflate.
- Re-test for leaks by gently pressing along the catheter and tubing; if leakage returns, stop and escalate. Tip: note the exact site of leakage for the clinician.
- If leaks persist or new symptoms appear (fever, increased pain, changes in urine color), contact a clinician immediately. Tip: keep a log of times and visuals for the medical team.
Safety tips and when to call a professional
Safety first. A catheter leak can introduce bacteria and increase infection risk. Do not attempt major repairs yourself or modify the system beyond simple reconnection and cleaning. If you observe blood in urine, fever, vomiting, or escalating pain, seek urgent medical help. Always inform your clinician about the leak’s location, timing, and any changes in urine characteristics. Consider scheduling a quick check with a home health nurse if you have ongoing concerns.
Prevention and long-term care to reduce leaks
Prevention centers on secure fittings, gentle handling, and regular checks. Ensure all connections are clean and tightly fastened, avoid pulling on the catheter, and keep tubing free of kinks. Position the patient so the drainage bag remains below bladder level, and check inflation volumes at routine intervals per clinician instructions. Document any changes in the system and communicate them to your healthcare team. Consistency in care reduces the likelihood of future leaks and supports safer home management.
Should catheter leak and device types: considerations for ongoing care
Different catheter types have varying risk profiles for leaks. Some designs include reinforced connectors and smoother tubing that resist pinching. If you notice recurrent leaks despite proper technique, discuss catheter alternatives or adjustments with your clinician. Understanding the device specifics helps tailor prevention and maintenance practices to your situation. The focus remains on keeping the passage clear and sterile, minimizing exposure to pathogens, and preserving skin integrity.
Steps
Estimated time: 30-60 minutes
- 1
Inspect all connections
Examine every junction for looseness or signs of wear. Clean the areas and reseal connections firmly with sterile technique if required. Ensure there is no moisture around the fittings that could indicate a developing leak.
Tip: Document the exact connection that was loose to inform your clinician. - 2
Straighten the tubing
Look for kinks and straighten the tubing to prevent backflow. Maintain a gentle curve that does not pinch the line, and keep tubing in a clean, unobstructed path.
Tip: Avoid placing tubing under furniture or heavy objects that could create pressure. - 3
Check bag position and attachment
The drainage bag should be below bladder level and secured to prevent tugging. Verify the outlet is open and the bag is draining; close clamps only when instructed by a clinician.
Tip: Use a stable stand to prevent accidental clamping or movement. - 4
Verify balloon inflation
Confirm the balloon is inflated to the prescribed volume. If inflation is uncertain, do not attempt to adjust; contact a clinician for guidance or replacement if needed.
Tip: Never force inflation beyond clinician-specified limits. - 5
Re-test for leaks
With the system closed, slowly apply light pressure along the catheter and tubing to see if leakage resumes. If leakage occurs at a new site, stop and report it immediately.
Tip: Keep a log of leak sites and times for your clinician. - 6
Escalate if needed
If leaks persist after these steps or you observe fever, severe pain, or rapid deterioration, seek urgent care and contact your clinician without delay.
Tip: Have all notes ready: when leak started, location, and affected equipment.
Diagnosis: Catheter leak observed at home (visible seepage from catheter, tubing, or bag junction)
Possible Causes
- highLoose connection at catheter or bag junction
- highKinked or pinched tubing
- highBalloon underinflation or damaged balloon
- mediumDislodgement or improper securement at insertion site
- lowFaulty drainage bag clamp or clogged line
Fixes
- easyTighten and reseal all catheter-to-tubing and tubing-to-bag connections.
- easyUnkink tubing; reposition to avoid bending and place bag below bladder level.
- mediumCheck balloon inflation against clinician guidance; replace catheter if balloon is defective.
- mediumEnsure securement at insertion site is appropriate; seek clinician assessment if looseness is suspected.
- hardReplace the catheter or adjust the setup under professional supervision if persistent leakage persists.
Questions & Answers
Is a catheter leak urgent or can I wait to see my clinician?
A catheter leak can indicate a risk of infection or device failure. If you’re unsure about the cause or if there are other signs like fever or severe pain, contact your clinician promptly or seek urgent care.
Catheter leaks can be serious. Contact your clinician promptly if you notice one, especially with fever or pain.
What are the most common causes of catheter leaks at home?
Loose connections, kinks in tubing, and balloon-related issues are the typical culprits. Identifying the exact site helps guide safe, effective fixes.
Most leaks come from loose connections, kinks, or balloon problems. Find the source to fix it safely.
Can I fix a leak myself or do I need a clinician right away?
You can perform basic checks and reconnections if you are trained and comfortable. If the leak persists, or you’re unsure about any step, contact your clinician for guidance or arrange a home visit.
You can handle basic checks, but if it keeps leaking, call your clinician.
When should I seek emergency care for a catheter leak?
Seek emergency care if you have fever, severe pain, rapid deterioration, or confusion, or if there is pus or blood in the urine. These could signal an urgent infection or device complication.
Go to emergency care if you have fever, severe pain, or blood in urine.
How can leaks be prevented in the long term?
Secure all connections, avoid bending tubing, monitor balloon inflation as instructed, and perform regular checks. Keeping a clean, organized setup reduces leak risk.
Prevent leaks with secure connections, gentle tubing, and routine checks.
Will a catheter leak always require replacement?
Not always, but persistent or recurrent leaks may require catheter assessment or replacement. Your clinician can determine the best course based on device type and symptoms.
Replacement is not always needed, but persistent leaks require clinician assessment.
Watch Video
Main Points
- Inspect connections first when a leak is noticed
- Kinks and balloon problems are common leak causes
- Call a clinician if leaks persist after basic fixes
- Prevent leaks with securement and routine checks
