Troubleshooting Brain Fluid Leak Symptoms
Urgent, actionable steps to recognize brain fluid leak symptoms, differentiate from other headaches, and know when to seek professional care. Learn a safe, structured troubleshooting approach from Leak Diagnosis.
CSF leak symptoms are typically marked by orthostatic headaches and clear nasal drainage, often following head trauma or sinus procedures. If you notice these signs, seek urgent medical evaluation. Diagnosis usually requires imaging and fluid tests to confirm a brain-fluid leak.
What is a CSF leak and why brain fluid symptoms matter
A cerebrospinal fluid (CSF) leak happens when the fluid surrounding the brain and spinal cord escapes through a tear or hole in the skull base or around the spinal canal. In medical terms, this can manifest as the symptom cluster clinicians describe as leak in brain fluid symptoms. The Leak Diagnosis team emphasizes that early recognition matters: CSF leaks can lead to serious infections like meningitis if not evaluated promptly. This section explains how leaks arise—from head injuries and certain medical procedures to spontaneous changes in pressure—and why understanding the signs is crucial for homeowners and DIY enthusiasts who may notice subtle changes after a fall, surgery, or sinus work. Reading this guide will help you differentiate common headaches from those linked to CSF leaks and prepare you for safe, informed conversations with healthcare providers.
Recognizable signs and symptoms of a CSF leak
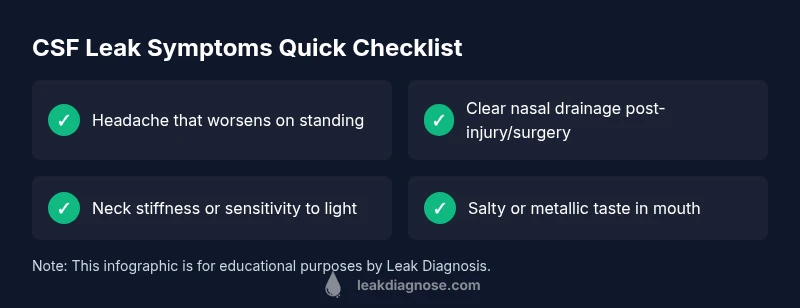
Leaking brain fluid doesn’t always look the same, but certain signals tend to cluster together. The classic red flag is a headache that gets worse when you stand up or sit upright and improves when you lie down. You may also notice clear, thin nasal drainage that increases with posture or bending over, a salty or metallic taste in the mouth, neck stiffness, sensitivity to light, or a persistent runny nose after head trauma or sinus surgery. Some people report muffled hearing, a change in balance, or an itchy, watery eye feeling. It’s important to treat these symptoms as potential signs of a brain-fluid leak and seek medical advice, especially if they follow an injury, surgery, or dental work that involved the skull base. The presence of fever, neck stiffness with a severe headache, confusion, or new neurological symptoms requires immediate emergency care.
How doctors diagnose a CSF leak
Clinicians approach a suspected brain-fluid leak with a combination of history, physical exam, and targeted tests. A hallmark lab test is beta-2 transferrin, a protein found almost exclusively in CSF, used to confirm CSF in nasal or ear drainage. Imaging studies—often MRI with specialized sequences or CT cisternography—help locate the leak source. In some cases, a dye or tracer is used during imaging to visualize CSF flow. Because symptoms can mimic other conditions (such as migraines or sinus issues), a careful evaluation by a healthcare professional is essential. Do not rely on home remedies alone; correct diagnosis guides effective treatment and reduces infection risk.
Diagnostic flow: symptom → diagnosis → solutions
When a patient reports orthostatic headaches and postural nasal drainage, clinicians pursue a step-by-step flow: confirm CSF in drainage, locate the leak, and assess brain protection risks. If a leak is confirmed, management ranges from conservative measures (hydration, bed rest, monitoring) to targeted interventions (epidural patches, surgical repair) depending on leak size, location, and patient health. Prompt referral to a neurosurgeon or ENT specialist is common. The goal is to stop leakage, seal the entry point, and prevent infections. In all cases, follow-up imaging and symptom tracking help ensure the leak has been resolved and that there are no ongoing issues.
Step-by-step home actions if you suspect a CSF leak
- Do not ignore warning signs. If you develop a sudden, severe headache after head trauma, fever, neck stiffness, or changes in consciousness, seek emergency care immediately. 2) Minimize activities that raise intracranial pressure (heavy lifting, straining, nose blowing) and stay hydrated to support general health. 3) Document your symptoms: note when they occur, what worsens or improves them, and any related nasal drainage or metallic taste. 4) If you’re able, collect a small sample of nasal drainage (only if advised by a clinician) for testing or bring a sample to your medical appointment. 5) Schedule a professional evaluation; do not rely on at-home fixes alone. 6) Follow your clinician’s plan, including any prescribed imaging or follow-up appointments, and report new symptoms promptly.
Prevention, safety, and when to seek help
Avoid activities that strain the head and neck after head trauma or nasal surgery and maintain good hydration as a general precaution. Use proper nasal hygiene and avoid forceful nose blowing, which can worsen a tear. If you notice persistent postural headaches, clear nasal drainage, or fever, treat this as urgent and contact a clinician promptly. Real-world prevention hinges on early detection, professional testing, and, when indicated, surgical repair to stop the leak and reduce infection risk.
Quick takeaways and practical next steps
- Be vigilant for orthostatic headaches and clear nasal discharge after head injury or sinus procedures. The phrase leak in brain fluid symptoms describes this pattern. - Seek urgent medical evaluation if symptoms are new, severe, or accompanied by fever or neck stiffness. - Rely on confirmatory tests (beta-2 transferrin, imaging) rather than self-diagnosis. - Follow through with specialist care; many leaks resolve with targeted treatments and careful follow-up.
Steps
Estimated time: Estimated total time: 60-90 minutes
- 1
Assess red flags and seek urgent care
If you experience a sudden, severe headache after trauma, weakness, confusion, fever, or neck stiffness, go to the ER immediately. Early evaluation can prevent complications like meningitis.
Tip: Do not wait for symptoms to worsen; emergency signs require rapid action. - 2
Limit activities that raise pressure
Avoid heavy lifting, straining, or nose blowing. Rest when possible and stay hydrated to support overall health while awaiting evaluation.
Tip: Gentle movement like light walking is usually safer than vigorous activity. - 3
Document symptoms methodically
Keep a log of when headaches occur, their severity, associated drainage, and any visual or sensory changes. This helps clinicians identify patterns.
Tip: Note posture-related changes and triggers to share with your clinician. - 4
Collect or present test information
Bring any prior imaging reports, notes from previous ENT or neurology visits, and a list of medications you’re taking for a smoother evaluation.
Tip: Prepare questions in advance to maximize your appointment time. - 5
Undergo recommended tests
Your clinician may order beta-2 transferrin testing on nasal drainage and imaging studies to locate the leak source.
Tip: Ask about test timing and what results mean for your plan. - 6
Follow through with treatment and follow-up
If a repair is indicated, understand the risks, expected recovery, and required follow-up imaging to confirm sealing of the leak.
Tip: Adhere to post-treatment instructions to reduce recurrence risk.
Diagnosis: Headache that worsens with standing or sitting, plus clear nasal drainage after head trauma or sinus surgery
Possible Causes
- highTraumatic skull base fracture or head injury
- highPostoperative CSF leak after nasal/sinus or intracranial surgery
- mediumSpontaneous CSF leak in susceptible individuals
- lowNasal infection or other non-CSF nasal drainage
Fixes
- easySeek urgent medical evaluation for confirmation with beta-2 transferrin and imaging
- mediumUndergo MRI or CT cisternography to locate the leak
- hardFollow specialist treatment, which may include conservative care or surgical repair
Questions & Answers
What are the most common brain fluid leak symptoms to watch for?
Common signs include orthostatic headaches that worsen when standing, clear nasal drainage, and neck stiffness. Some people notice a salty taste or hearing changes. These symptoms warrant medical evaluation to confirm whether a CSF leak is present.
Key signs include posture-related headaches and clear nasal drainage—see a clinician promptly for confirmation.
Is a CSF leak always serious or emergency-worthy?
A CSF leak can be serious due to infection risk, but not all cases require immediate surgery. Urgent evaluation is advised, especially after trauma or persistent symptoms.
Urgent care is recommended, especially after trauma or lingering symptoms.
What tests diagnose a CSF leak?
Doctors use beta-2 transferrin testing on drainage and imaging studies such as MRI or CT cisternography to locate the leak and plan treatment.
Tests include a beta-2 transferrin test and brain imaging to locate the leak.
Can a CSF leak be treated at home?
Home care is limited to supportive measures like avoiding activities that raise pressure and staying hydrated; definitive diagnosis and treatment require medical care.
Home care helps only alongside professional evaluation and treatment.
What is the typical course after diagnosis?
Treatment may range from conservative management to procedures that seal the leak. Regular follow-up imaging helps ensure the leak is closed and to prevent recurrence.
Treatment varies; many cases improve with proper care and follow-up.
Watch Video
Main Points
- Identify posture-related headaches and clear drainage as potential CSF leak signs
- Seek urgent evaluation for confirmation tests and imaging
- Follow through with expert treatment to reduce infection risk
- Keep thorough symptom records for accurate diagnosis